When using a transcutaneous pacemaker, it is important to remember that the pacing stimulus can cause an artifact on the ECG. This artifact is sometimes confused for a QRS complex. Also, the pacing of the chest wall muscles can be misinterpreted as a pulse. A “real” QRS complex will have a T wave.
In this strip, the underlying sinus bradycardia is uninterrupted across the strip. The rate is very slow – in the 30’s.
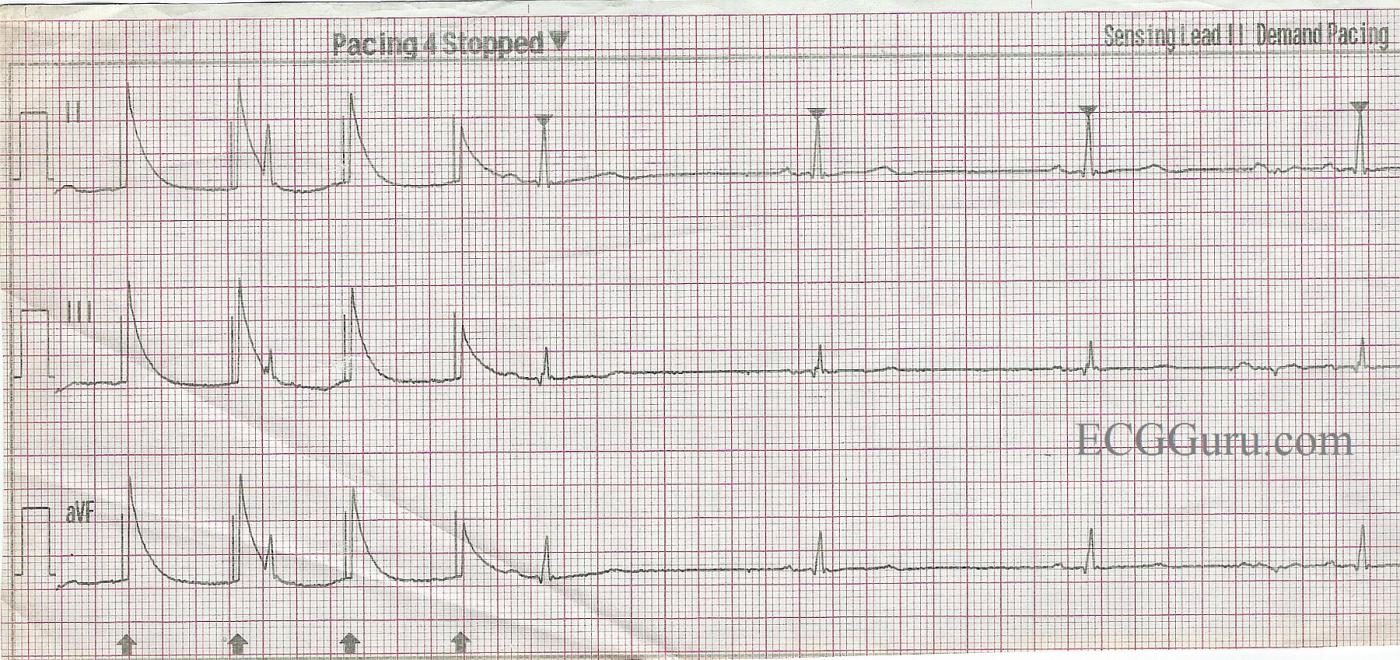
At the beginning of the strip, there are four pacing stimuli, with artifact. The pacemaker is in fixed mode. It does not sense the normal QRS that occurs after the second pacing stimulus. There is failure to sense AND failure to capture. Apparently, the pacing is stopped, then the pacer is set to “demand” mode. The pacemaker is sensing the patient’s native beats, but not pacing. It is likely that the rate and/or the MA, or milliamps, need to be increased to achieve pacing with capture.
This is a good ECG to illustrate the artifact that is possible with transcutaneous pacing, and remind your students not to assume the patient is being paced. The patient’s clinical signs (skin perfusion, blood pressure, mentation) should be used to determine whether the rate is adequate.
All our content is FREE & COPYRIGHT FREE for non-commercial use
Please be courteous and leave any watermark or author attribution on content you reproduce.


Comments
False Capture Pacing Spikes
It is tempting to say that the first 4 complexes show pacer spikes with capture — but that is NOT what is happening … Despite those large deflections occurring ~ 0.04 second after the pacing spikes, this does not represent ventricular capture. Instead, it shows “phantom QRS complexes” of the phenomenon of “false capture”. This phenomenon is wonderfully explained by Tom Bouthillet. Tom’s classic 2008 post is well worth reading. As Dawn emphasizes — true pacing capture is manifest by production of both a QRS and T wave, and we do not have that here.
Ken Grauer, MD www.kg-ekgpress.com [email protected]